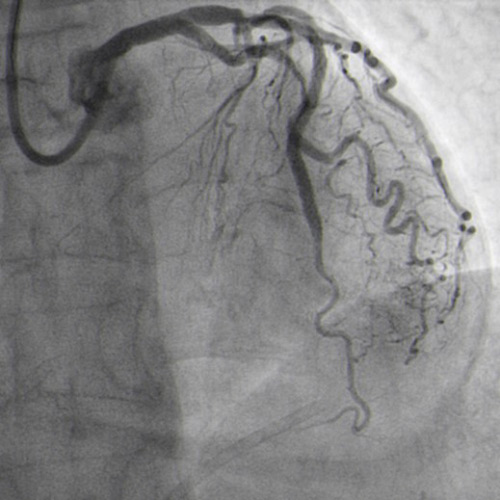
  The trial is registered under, with number NCT00819923. Informed written consent was obtained from every patient after explanation of the trial protocol the protocol was approved by the ethics committees of the participating centers. The trial was initiated by the investigators and conducted according to the ethical guidelines of the 1964 Declaration of Helsinki, as revised in 2013. Follow-up was planned at 12 months, and yearly thereafter through 7 years. Early PCI entailed undertaking coronary angioplasty and stent implantation within 12 hours of symptom onset in patients presenting with STEMI, and within 72 hours in those presenting with non-ST-segment elevation ACS (NSTEACS). Briefly, BASE ACS trial was a prospective single-blinded randomized (1:1) trial in which 827 patients who underwent early PCI for ACS received either titanium-nitride-oxide-coated or everolimus-eluting stents. The trial design was described previously. In a post-hoc analysis of the trial, we explored the incidence, predictors, and long-term outcome of poor initial Thrombolysis In Myocardial Infarction (TIMI) flow in patients treated by early PCI for ACS. BASE ACS trial, showed non-inferiority of titanium-nitride-oxide-coated versus everolimus-eluting stents, for the primary endpoint of major adverse cardiac events (MACE) in patients with ACS at mid- and long-term follow-up. 
Several reports demonstrated safety of titanium-nitride-oxide-coated stents in unselected cohorts, and in randomized trials of patients with ACS. Yet, predictors and outcome of poor initial TIMI flow in patients treated by early PCI for acute coronary syndrome (ACS) remain unclear. Predictors of initial infarct-related artery patency in patients presenting with STEMI were previously reported. Previous studies demonstrated that infarct-related artery patency early before primary percutaneous coronary intervention (PCI) is associated with a better immediate angiographic outcome, and independently predicted better survival at mid-term follow-up, in patients presenting with acute ST-elevation myocardial infarction (STEMI). Definite ST occurred more in patients with poor, versus good, initial TIMI flow, mainly driven by difference in early events. Predictors of poor initial TIMI flow included presentation by ST-elevation myocardial infarction, and target vessel other than left anterior descending artery. This was driven by more frequent early events (30 days) ( p = .036) late/very late events were comparable ( p = 1.0). Definite ST was more frequent in patients with initial TIMI 0/1 flow (3.6% versus 1.5%, respectively, p = .048). Individual endpoints were comparable ( p > .05 for all). 
MACE rate was comparable between the 2 subgroups (14% versus 15.9%, in patients with poor versus good initial TIMI flow, respectively, p = .46). Presentation by ST-elevation myocardial infarction and target vessel other than left anterior descending artery predicted initial TIMI 0/1 flow. Of 827 patients enrolled, 279 (33.7%) had initial TIMI 0/1 flow. Propensity score-matched analysis was performed. Stent thrombosis (ST) was adjudicated according to the criteria of definite ST described by the Academic Research Consortium. The primary endpoint was major adverse cardiac events (MACE): a composite of cardiac death, non-fatal myocardial infarction or ischemia-driven target lesion revascularization. Poor initial TIMI flow was defined as baseline TIMI flow grade 0/1 at the initial coronary angiography. We performed post-hoc analysis of a randomized trial of patients presenting with ACS who received 2 comparative stents. We explored the predictors and outcome of poor, versus good, initial TIMI flow in patients with acute coronary syndrome (ACS). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
